Streamlined Claims Processing from Intake to Resolution
Everblue’s Claim Management solution automates the intake, review, and resolution of claims across complex programs. Our platform reduces processing time while improving accuracy and transparency.

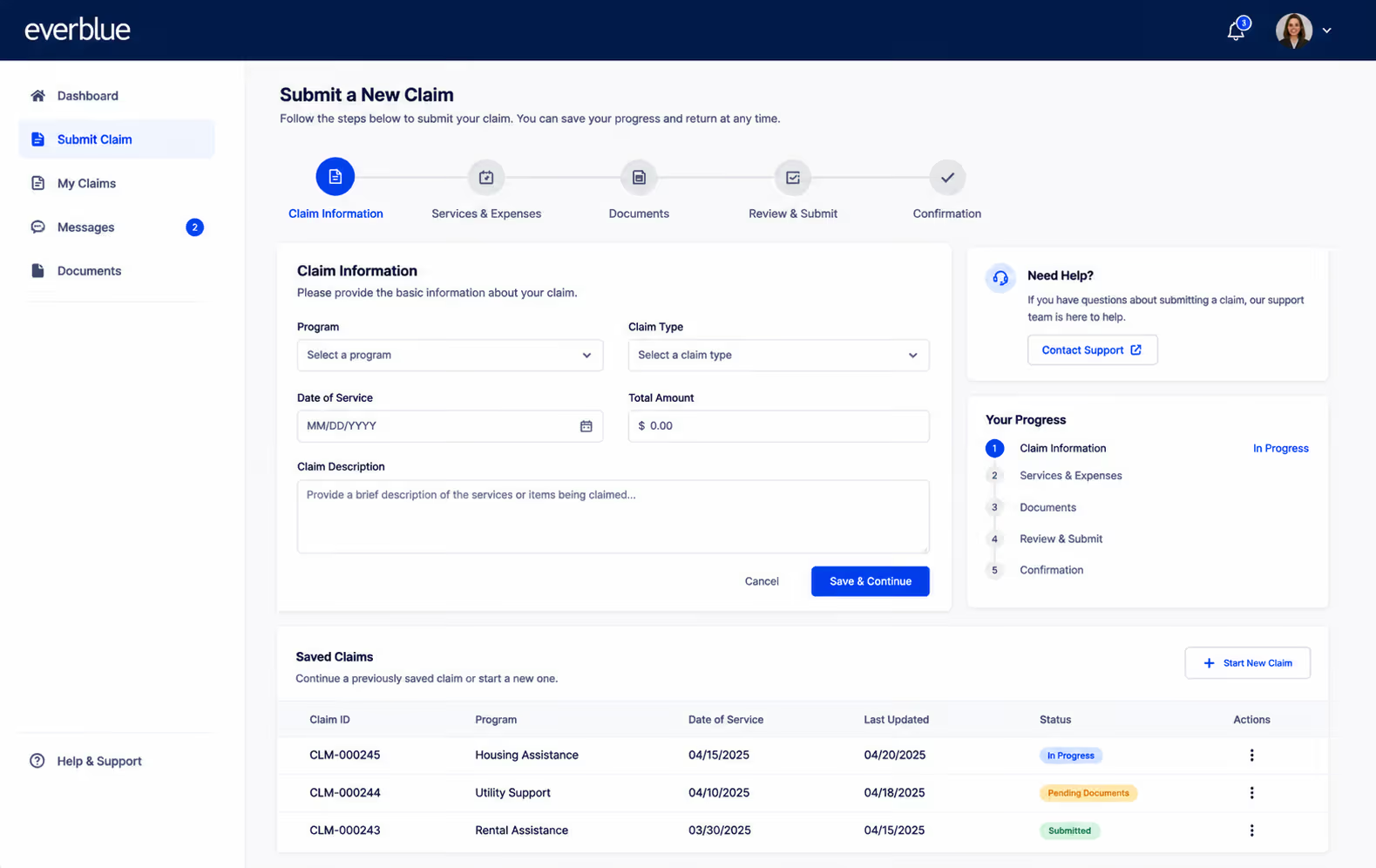
Key Capabilities
- Online claim submission portals
- Automated validation and review workflows
- Secure documentation handling
- Status tracking and notifications
- Reporting and audit support

Who It’s For
- Program administrators
- Government agencies
- Public benefit programs

Outcomes
- Faster claim resolution
- Reduced administrative burden
- Improved accuracy and compliance
- Higher stakeholder satisfaction
.webp)
.webp)
.webp)



.avif)

